
Are you looking for the PHAC guidance document for practitioners?
Updated October 30, 2025
NCCID Disease Debriefs provide Canadian public health practitioners and clinicians with up-to-date reviews of essential information on prominent infectious diseases for Canadian public health practice. While not a formal literature review, information is gathered from key sources including the Public Health Agency of Canada (PHAC), the USA Centers for Disease Control and Prevention (CDC), the World Health Organization (WHO) and peer reviewed literature.
Questions, comments and suggestions regarding this debrief are most welcome and can be sent to nccid@umanitoba.ca.
What are Disease Debriefs? To find out more about how information is collected, see our page dedicated to the Disease Debriefs.
What are important characteristics of Lyme disease?
CAUSE
Lyme disease is a bacterial infection caused by Borrelia burgdorferi. It spread through the bite of infected ticks. Ticks attach to any part of the human body but are often found in hard-to-see areas. In most cases, the tick must be attached for at least 24 hours before Lyme disease can be transmitted.
Most humans are infected through the bites of immature ticks called nymphs. Nymphs are tinny (less than 2 mm).
SIGNS AND SYMPTOMS
Incubation period: 3-30 days after tick bite.
Early signs and symptoms include rash sometimes like a bull’s eye rash (Erythema migrans rash), fever, chills, headache, fatigue, muscle and joints aches and swollen lymph nodes.
If untreated, severe symptoms include severe headaches, facial paralysis (Bell’s Palsy), muscle, joint, tendon and bone aches, heart disorders, neurological disorders.
- Government of Canada-Symptoms of Lyme disease
- CDC-Lyme disease-Signs and Symptoms of Untreated Lyme disease
CLINICAL MANIFESTATIONS
Typically, clinically symptoms are three pronged.
a) Early localized Lyme disease (within a month)– symptoms include fever, arthralgias, myalgias, headache, the presence of a single, localized skin lesion known as erythema migrans (EM)
b) Early disseminated Lyme disease (less than 3 months)– symptoms such as fatigue and general weakness, cutaneous signs, typical cardiac complications include atrioventricular block, tachyarrhythmias, myopericarditis and myocardial dysfunction, neurological symptoms are aseptic meningitis, radiculopathy, encephalopathy, cranial neuropathy (especially facial nerve palsy), monomeutitis multiplex, subtle cognitive difficulties, motor and sensory radiculoneuropathy. Other manifestations are uveitis, keratitis, conjunctivitis, mild hepatitis, and splenomegaly.
c) In the case of Late Lyme disease (more than 3 months), if it remains untreated, it can last for months and years. Musculoskeletal symptoms could develop such as Baker’s cyst, chronic arthritis, asymetric oligoarticular arthritis (usually affecting knees), transient, migratory arthritis and effusion in one or multiple joints. Neurological symptoms may also be observed such as: subacute mild encephalopathy, affecting memory & concentration, chronic mild axonal polyneuropathy, manifested as distal paresthesias, radicular pain (less common), some rare ones include encephalomyelitis & leukoencephalopathy.
- Government of Canada-For Health Professionals-Clinical Manifestations
- Alberta Health-Lyme disease & tick surveillance in Alberta-Diagnosis and Laboratory Testing
Laboratory Testing:
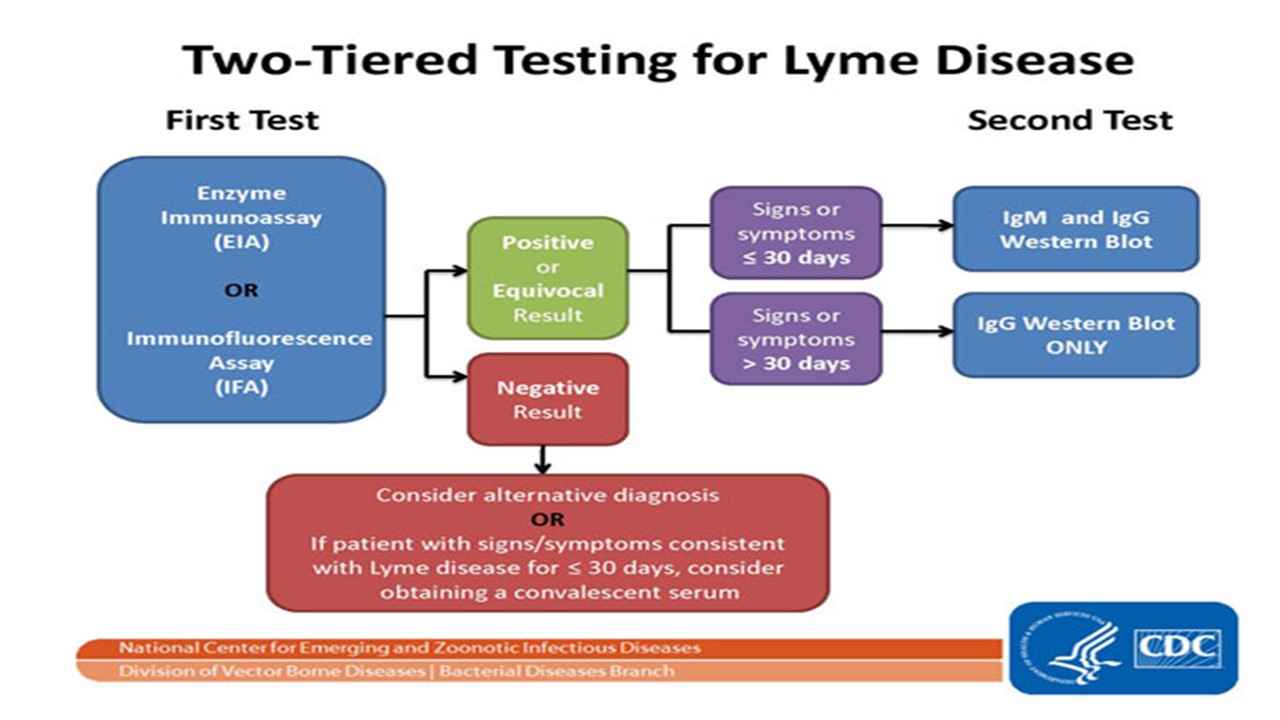
Two tiered serological testing for antibodies against bacterium causing Lyme disease is recommended.
a) An enzyme immunoassay (EIA) screening test
b) A confirmatory immunoblot (IB) test (if the EIA is positive or equivocal)
Only IgG testing should be performed (not IgM) on patients with Lyme disease for over a month.
Serological tests should not be performed as a test of cure & cannot be used to measure treatment response.
- Government of Canada-For Health Professionals-Lyme disease-Laboratory Testing
- New Brunswick-Office of the Chief Medical Officer of Health (Public Health)-Lyme disease-Brief reference for New Brunswick clinicians-Diagnosis and Testing
- CDC-Lyme disease-Diagnosis and Testing-Two-step Laboratory Testing Process
Treatment:
The treatment guidelines for early Lyme disease include (source: Government of Canada-For Health Professionals: Lyme disease-Treatment):
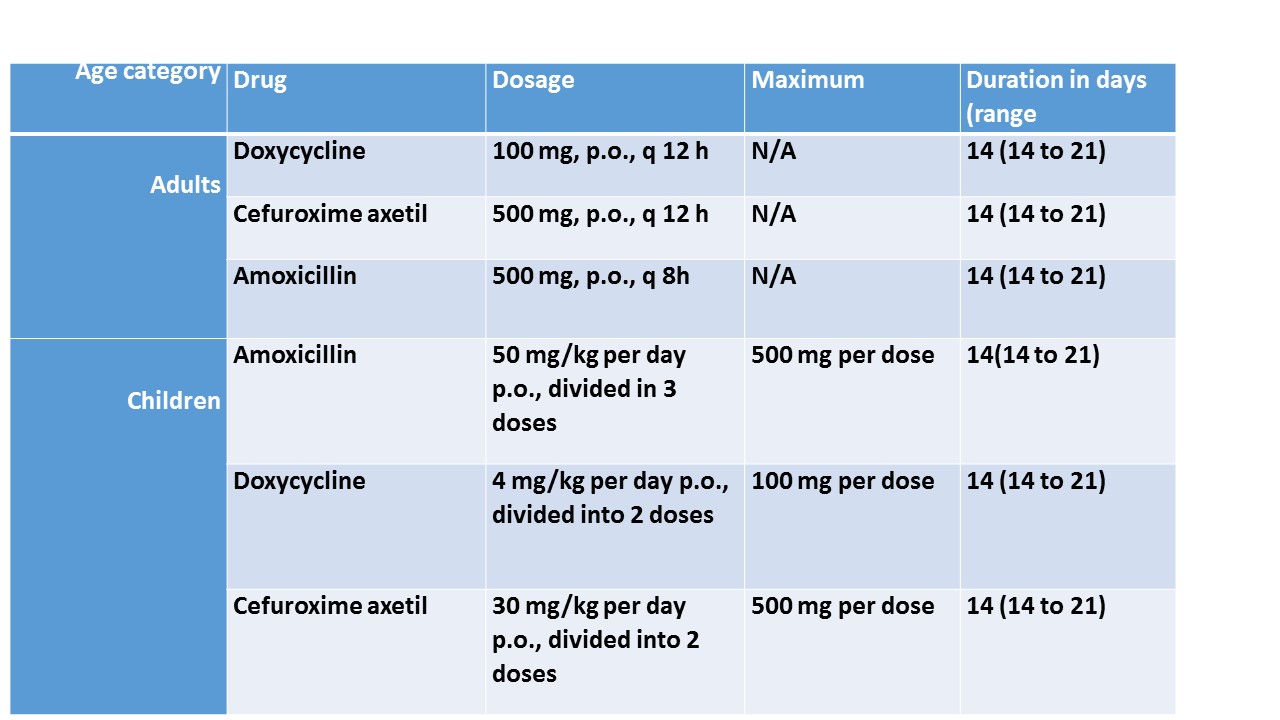
Important:
Doxycycline is contraindicated for children less than 8 years old and for pregnant or lactating mothers so the drug of choice is Amoxicillin in this case.
In cases where these are not drug of choice, patients are recommended to use macrolide (azithromycin, erythromycin, clarithromycin).
Prevention:
The best prevention strategy is to protect against tick bites, as there is no human vaccine currently available against Lyme disease.
Lyme disease is not a contagious disease however, people with active Lyme disease should not donate blood as it can a medium of transportation.
- Government of Canada-Prevention of Lyme disease
- Government of Canada-For Health Professionals-Lyme disease-Prevention
- Government of Canada-Lyme disease prevention toolkit
- Nova Scotia-Communicable Disease Prevention and Control-Lyme disease
What is happening with current outbreak of Lyme disease?
A preliminary total of 5,239 human cases of Lyme disease were reported to the Public Health Agency of Canada in 2024, compared to 4,785 and 2,525 reported cases in 2023 and 2022, respectively. Of all cases reported in between January 1, 2022 and December 31, 2022, 2,093 (82.9%) were confirmed. Most of these cases were reported from Ontario (1,478), Quebec (586), and Nova Scotia (326). Nova Scotia reported the highest incidence at 32.0 per 100,000 population, which was nearly 5 times higher than the national incidence (6.5 per 100,000 population). The table below shows the number of confirmed and probable cases as well as incidence per 100,000 population of all reported cases of Lyme disease in Canada in 2022.
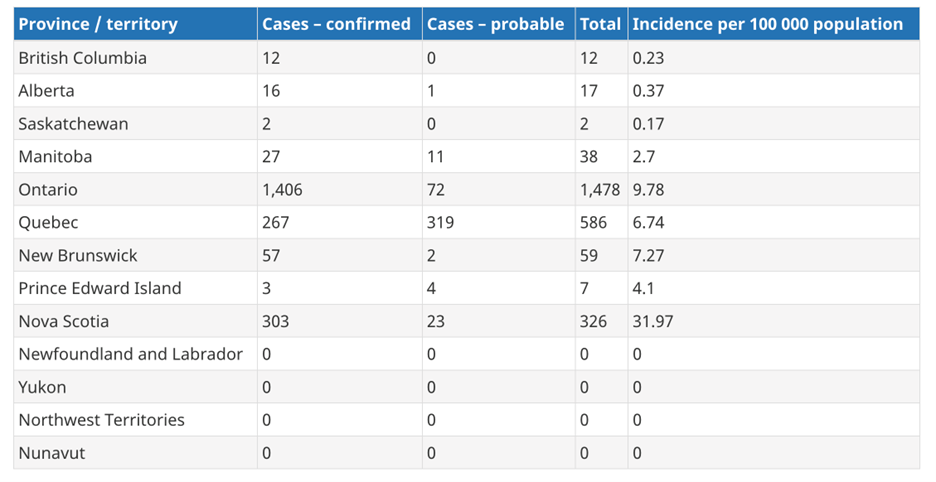
The Public Health Agency of Canada reports that the national incidence rate of Lyme disease has been rising since 2009, highlighting the need for ongoing prevention and awareness efforts.
What is the current risk for Canadians from Lyme disease?
The risk of contracting Lyme disease is very high across southern Canada during warm weather (Spring & Summer) and especially during outdoor activities such as golfing, hunting, camping, fishing & hiking. Surveillance data indicates that blacklegged ticks are spreading in eastern & central Canada.
What measures should be taken for a suspected Lyme case or contact?
CASE AND CONTACT MANAGEMENT
The Government of Canada has developed brief guidelines to help healthcare providers in the management and treatment of Lyme disease infection. These include signs, symptoms, diagnosis, laboratory testing, surveillance, prophylaxis, treatment.
Public Health Ontario has worked with other public health units and Public Health Agency of Canada to develop a Lyme disease case management tool companion guide which identify exposure location, improve case and contact management, provide case counseling, assist with disease management, obtain required data elements under the health protection and promotion act pertaining to the case and facilitate investigation documentation.
CASE DEFINITIONS
Government of Canada developed Lyme disease case definition in 2016 for confirmed case, probable case, and clinical evidence. Since 2009, Lyme disease has been nationally notifiable disease.
In March 2017, The Ministry of Health Long-Term Care Ontario published the provincial case definitions for Lyme disease.
- Ministry of Health and Long-Term Care Ontario-Provincial Case Definition for Lyme disease
- Manitoba Health, Seniors and Active Living-Epi Report-Manitoba Annual Tick-Borne Disease Report 2016
- British Columbia Centre for Disease Control-Lyme Case Definitions
INFECTION PREVENTION AND CONTROL
Government of Canada and provincial authorities have laid out guidance to prevent infection from Lyme disease.
